Calendar Icon
Apr 23, 2018
Person Bust Icon
By Karl Vogel
![]() RSS
Submit a Story
RSS
Submit a Story
Starting from “ground zero,” four biological systems engineering students turned their senior design capstone project into a device that could help first responders save more lives in emergency situations – and also help build their resumes.
The team of Catelyn Evans, Hunter Miller, Nicholas Seier and Alexis Woodward was assigned to develop a modified laryngoscope that could help medical personnel in the field better perform endotracheal intubations. In out-of-hospital settings, only two-thirds of medical personnel are successful on the first attempt of inserting a breathing tube into the trachea (windpipe) to maintain an open airway.
To begin, In the team needed a crash course in intubation.
“We started at ground zero. We knew nothing,” Woodward said.
“We had to watch videos online to learn what intubation was,” Evans added.
They also considered that many medical personnel – doctors, paramedics, EMTs (emergency medical technicians), etc. – in lower-populated areas might not have the experience or training necessary. In the field, a device that makes intubating a patient simpler could save more lives.
“There’s just so many more complications (in a field intubation),” Evans said. “A lot of times there’s fluid or other things blocking the airway, and that makes it difficult to see the path the tube has to take.”
Their research included looking at the many laryngoscopes used to perform intubations and the various methods used. The team had its first design completed before the end of the fall semester and manufactured it on a 3-D printer early in the spring semester.
Early this semester, the team met with the firefighters and paramedics at Lincoln Fire and Rescue (LFR) Station 2 – just a short walk from Chase Hall.
“We went over there before we printed up our first design to get some hands-on experience with intubation and hear first-hand what some of the issues are and how they can be remedied. We took that into account with our design,” Miller said.
Capt. Ryan Murphy said the firefighters and paramedics were impressed with the engineering students.
“When I first talked to the students, I assumed they knew all about intubation, but when we took them into the station, we found out how little about our side of it they knew,” Murphy said. “But they asked some awesome questions about the problems we encounter.”
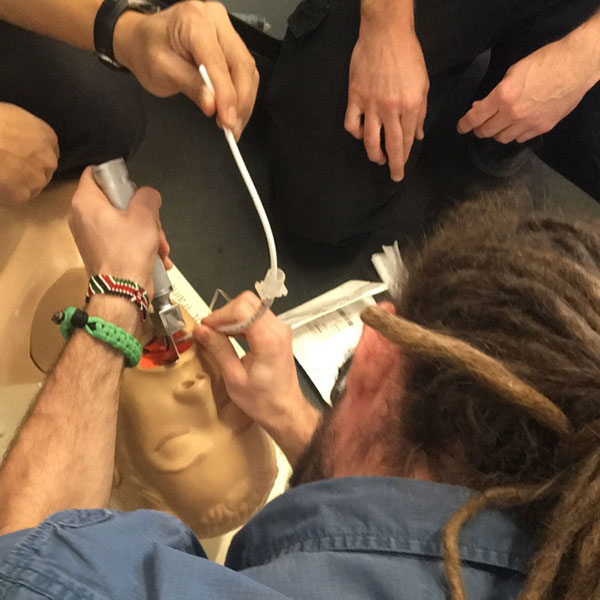
Testing the device on an LFR mannequin, the students learned they didn’t know enough.
“Having never done that ourselves, being able to go to the paramedics and learn, it was eye-opening,” Seier said. “It takes quite a bit of force to displace all the soft tissues in the mouth.”
Using the glottis (the opening between the vocal chords) as a guide is of paramount importance in performing an intubation. After working on the mannequins, Evans said, the team realized this would be trickier in the field.
“When we tried to position the scope, just moving it with enough force is hard because you’re trying to move dead weight,” Evans said. “Sometimes, you wouldn’t want to lift or move a patient’s head if they have a neck injury, and that could make visualization difficult.”
Murphy and his crew liked the device, but told the students it could still be improved.
“We found a few hiccups, things that possibly need to be changed, based on what we encounter,” Murphy said.
Armed with feedback from the paramedics, the students went back to work.
After modifying the design and printing a new device, they took it back to the fire station and got a positive response to the prototype. That, the team members said, was a relief.
“They were very impressed,” Woodward said. “It helped to verify that we are capable of solving problems in the world – finding solutions from what we know, what we’ve been taught and what we’ve gained.”
Currently, NU Tech Ventures is reviewing the students’ design to possibly pursue a patent. That, would be an unexpected feather in their caps and a possible gold star on a resume, Woodward said.
Submit a Story
